COVID-19 Buildings & tents layout design guidelines by World Health Organization
Download the WHO standard screening layout for converted buildings and tents.
Hospitals and other health-care facilities play a critical role in national and local responses to emergencies, such as the COVID-19 epidemics. This document provides information on how these facilities can fulfill this role (28).
For the anticipation, early detection and containment response, from the introduction to the localized transmission phase, the following are recommended:
- Foresee a proper screening system at all levels of the public health system to enable early detection of potential suspected cases. This should include temporary isolation capacity, trained staff, protocols and all needed supplies.
- Designate health facilities to provide the adequate level of care, which most probably will be hospitals with available intensive care units, and set up the correct IPC and engineering measures.
- Define a clear referral pathway for suspected and confirmed cases with dedicated ambulance service to facilitate referrals from primary health centres to identified treatment facilities.
- Develop a control and mitigation plan.

This section suggests practical advice, recommendations, technical guidance and minimum requirements for setting up and operating a specific SARI screening and related waiting room, including the standards needed to repurpose an existing building into a SARI screening.
Identification, selection and survey of screening sites
The choice of a site will determine future problematic issues that could be encountered, such as infiltration, drainage, access, extension and acceptance. Take the necessary time to carefully choose the site that is as adequate as possible, rather than the first one seen.

It is important to know the average daily patient influx in order to properly size the waiting room and avoid possible overcrowding, even during the daily influx peak, which may increase the risk of nosocomial infections.
Location criteria
- Ensure the site is as close as possible to the main entrance of the health facility in order to centralize all entrances.
- Ensure good access for patients, visitors and staff, with guaranteed security.
- Aim for a unidirectional flow for all patients and visitors accessing the health facility.
- Avoid all flood areas and choose a site at least 30 m away from rivers or other bodies of water

Ground characteristics
- Ensure the site is flat and level.
- Ensure the site is geologically stable and consolidated, preferably without organic or stony material.
- Ensure the site is easy to dig, without the danger of landslides, and with the capacity for drainage.
- Avoid areas with a high groundwater table.
- Ensure the site is of sufficient size to extend the waiting room and triage area if necessary.

Meteorological characteristics
- Be aware of seasonal periods affecting the construction (e.g. rainy/dry periods). Be able to adjust the design to accommodate different climatological conditions.
- Take into account prevailing winds for the control of smoke and odours.
- Take into account sun orientation for improved shadow zones.

Existing resources
• Consider using permanent buildings or unused existing wards.
• Evaluate water resources in the area, with special focus on the analysis of capacity, quality and availability.
• If available, have the option to connect to local basic services for water, electricity and communications.

Download the WHO standard screening layout for converted buildings and tents.
Screening basic layout principles
The proposed layout is based on the standard screening setting endorsed with proper ventilation infection, prevention and control measures. The following assumptions are behind this layout:

- Protocols for patient screening (including the designation of screening areas) and for patient traffic flow within and in the vicinity of the hospital are available.
- Staffing is provided for newly designated hospital areas, such as the new screening area and isolation room.
- The hospital applies screening criteria with a view to admitting the most critically ill patients and treatable epidemic patients. In some circumstances, health authorities may require a health facility to focus on providing health services to non-epidemic patients and to refer epidemic patients elsewhere.

This document aims to present different structural approaches to set up a waiting room and triage area specifically adapted for COVID-19 in the following situations:
• New-construction concrete building or semi-permanent structure; the standards proposed here can also be used to repurpose existing buildings.
• Large tent (> 100 m2), as commonly used in emergency settings by humanitarian actors, institutions and United Nations agencies to set up warehouses and high-capacity shelters.
• Standard-sized tent (about 45 m2), as commonly used by humanitarian actors, institutions and United Nations agencies for emergency responses.

Screening in new health-care facilities
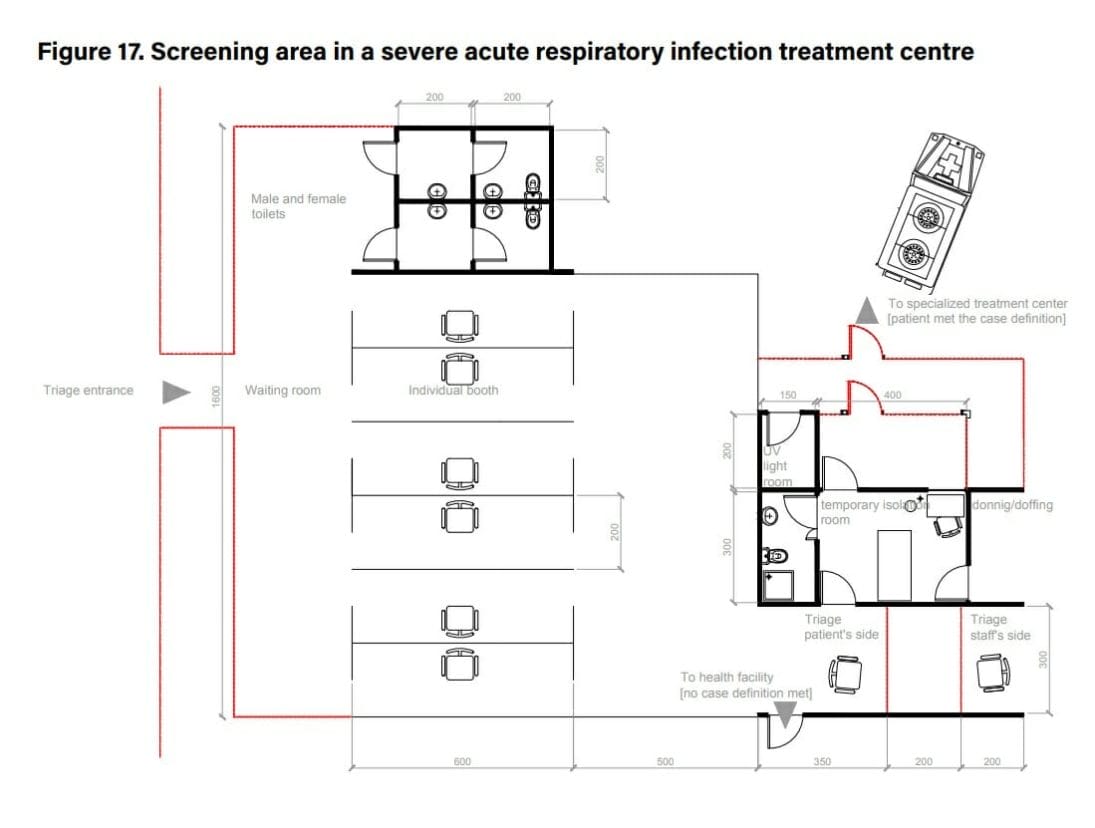
Screening is divided into two distinctive zones: one zone for staff and one zone for patients (Figures 17–19). A distance of 2 m between staff and patients is required.1
Double fencing or a Plexiglas barrier can be used for the separation. Separate handwashing points (soap/water) are required for patients and staff.

The screening building could be a temporary structure, a repurposed existing building, or a simple tent (see Annex 16). Natural ventilation and exhausted air dilution should be ensured. Note that staff should not wear masks in the screening area, except when in contact with patients.
COVID-19 buildings screening area
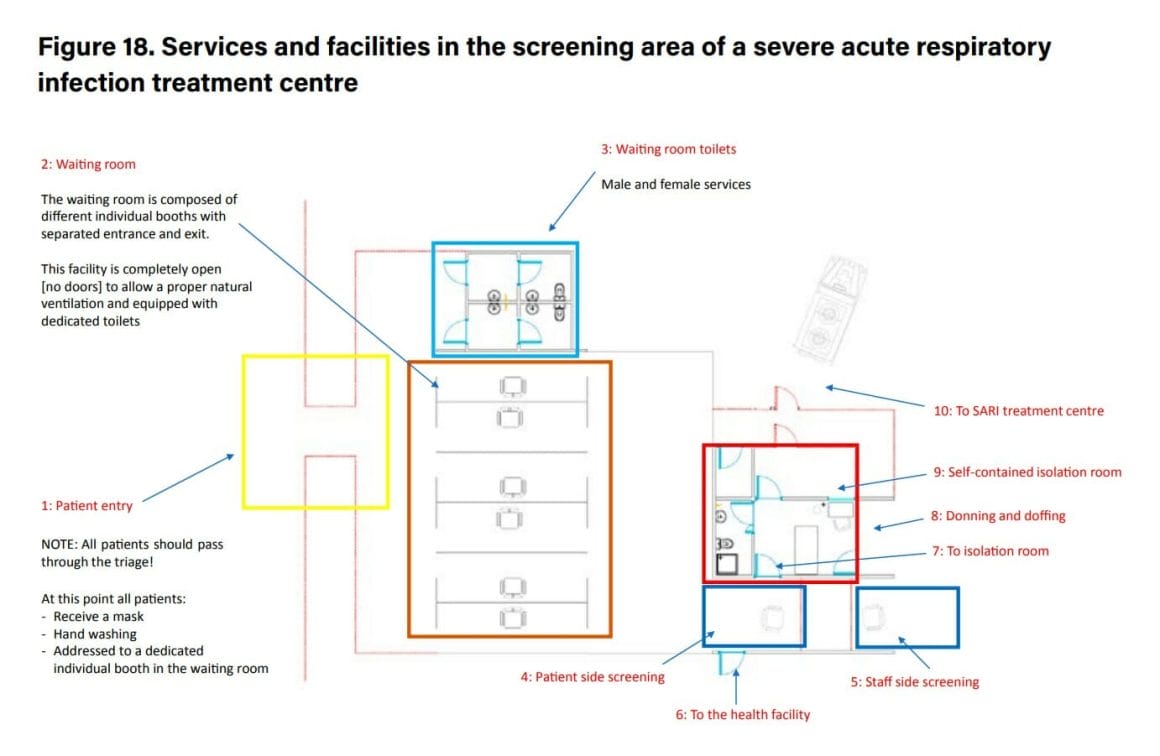
COVID-19 buildings services and facilities
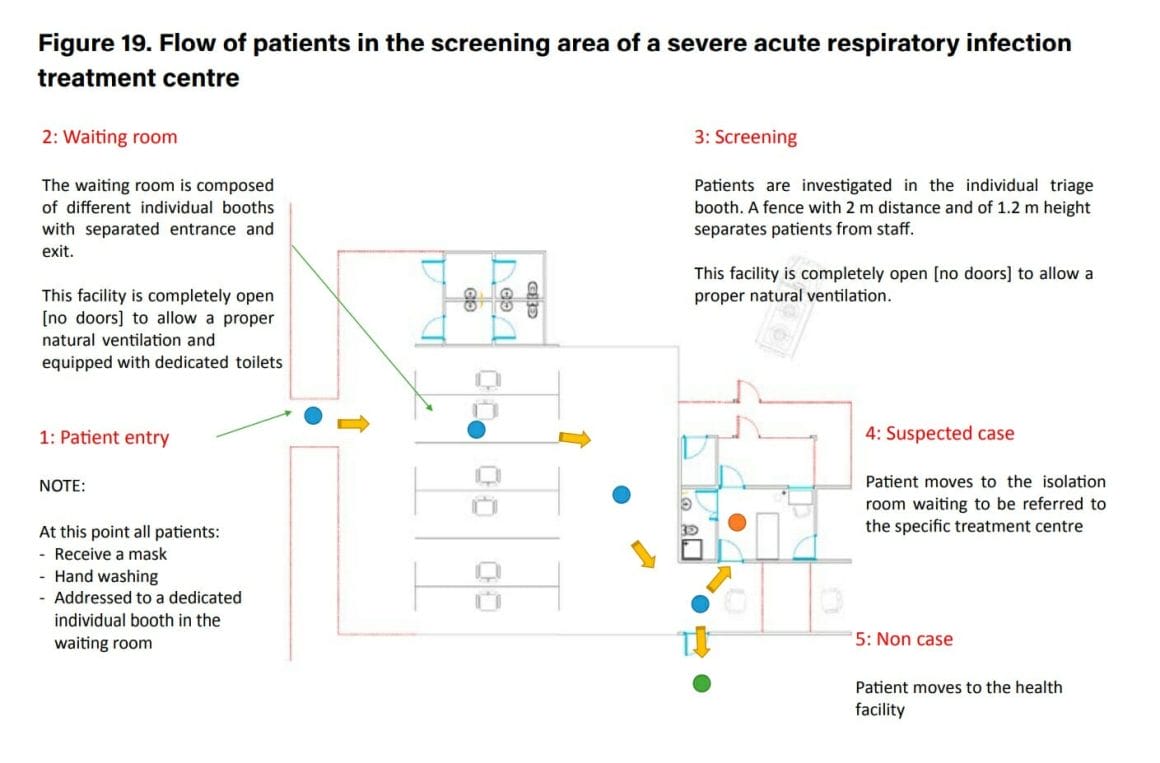
COVID-19 buildings flow of patients
Waiting room
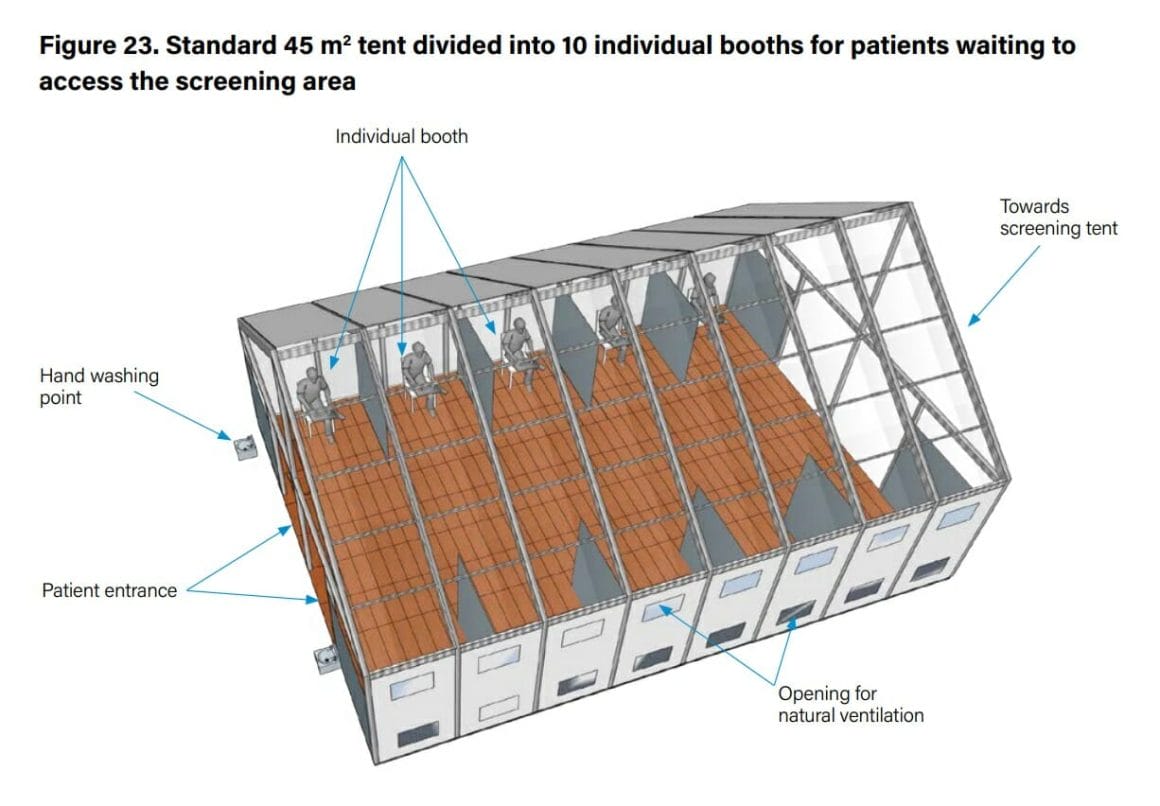
The waiting room should be composed of individual booths open on both sides to ensure proper natural ventilation. Each booth should be clearly identified and labelled to avoid mistakes and allow patient flow. Booths should be cleaned and disinfected after each patient to avoid nosocomial infections. If individual booths are not available, ensure a distance of at least 2 m between patients.2

Isolation room
The isolation room is a temporary area for a person suspected of being infected to wait for an ambulance or referral. If there is no isolation capacity, an ambulance could be held in standby near the screening area in order to allow rapid referral.
If needed, sampling can be done in the temporary isolation room.

Establishing a screening area in a tent
The lack of an existing building to be repurposed or the need to set up a screening area as quickly as possible may lead to using a tent as this is quicker than building a semi-permanent structure and cheaper than building a concrete structure. It is essential to respect all the IPC requirements in terms of distance between patients and proper flows.

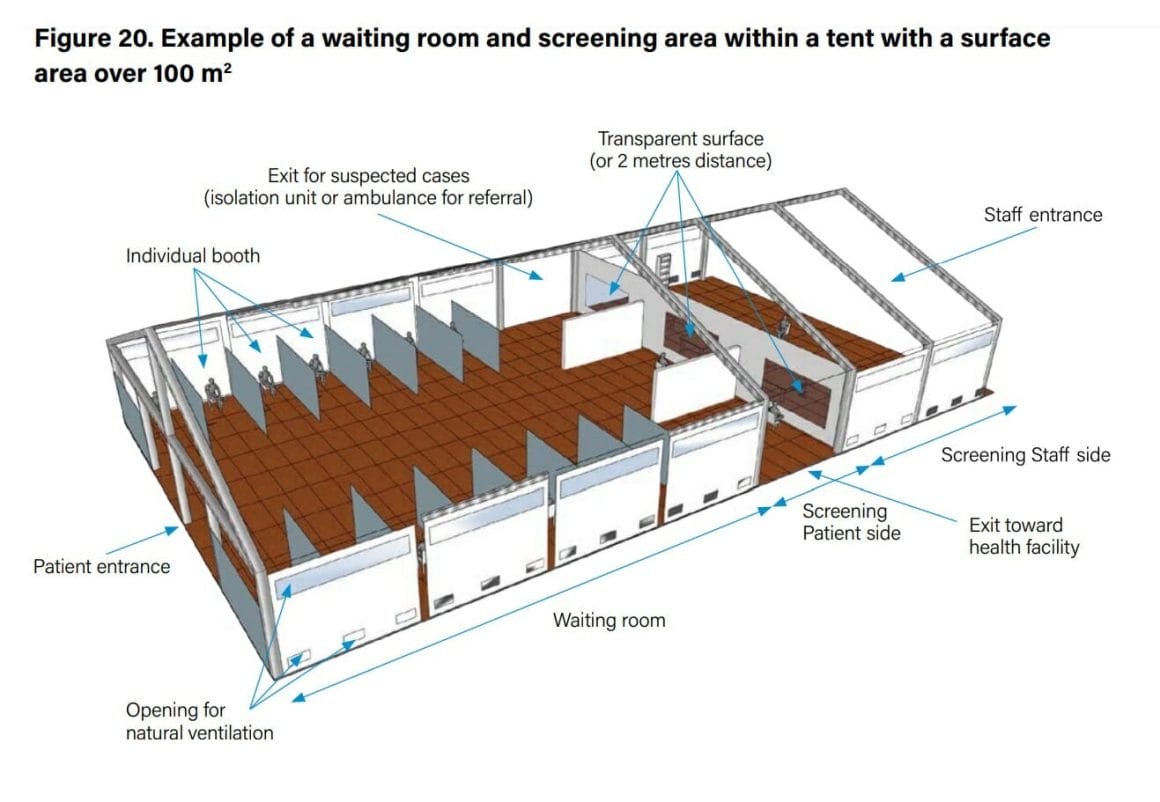
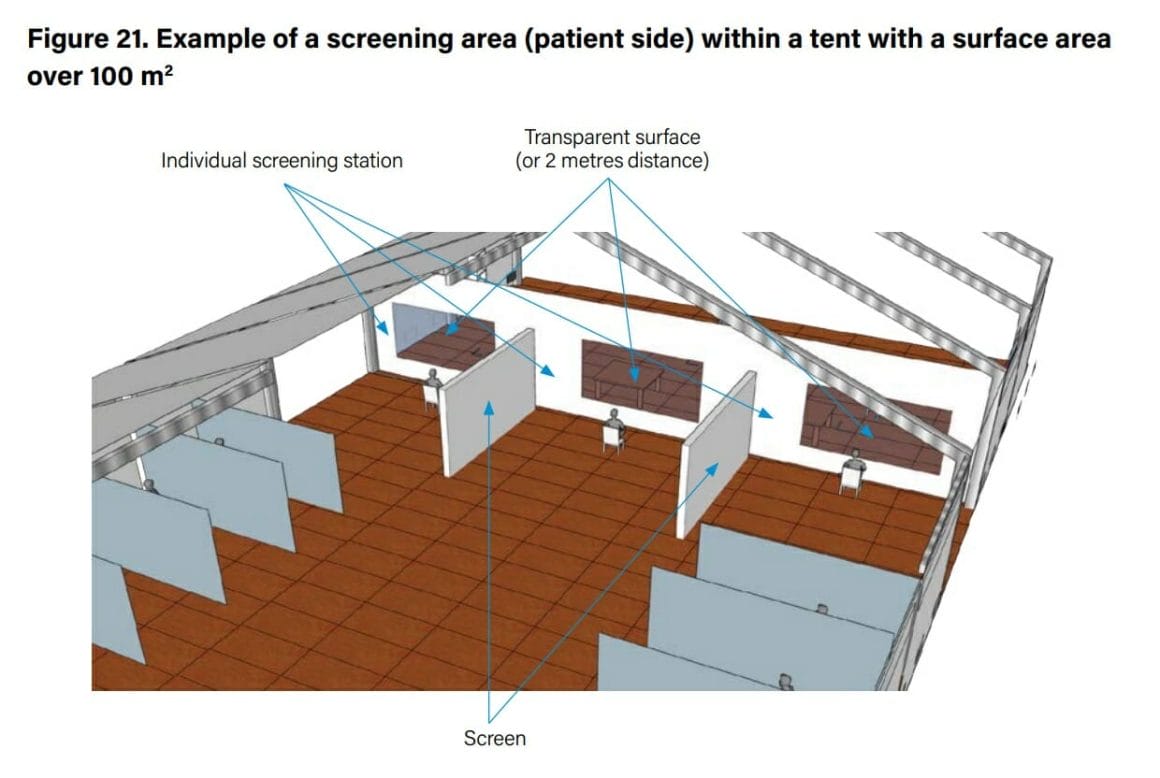
Figures 20 and 21 show examples of how a tent could be used to set up a waiting room and screening area. If a single tent with a surface area greater than 100 m2 is not available, then several smaller tents can be used and the waiting room space split between them, according to specific setting needs. Consider installing handwashing points at patient’s and staffs’ entrance and exit. Dedicated toilets for patients in the waiting room should be available, with a related handwashing point.

In cold-weather countries it is possible to replace natural ventilation with a mechanical or hybrid system with specific exhausted air treatment or a portable air filtration system, sized according to the capacity of the waiting room (airflow 60 l/s/person).
COVID-19 buildings and tents waiting room and screening area
COVID-19 buildings and tents waiting room and screening area

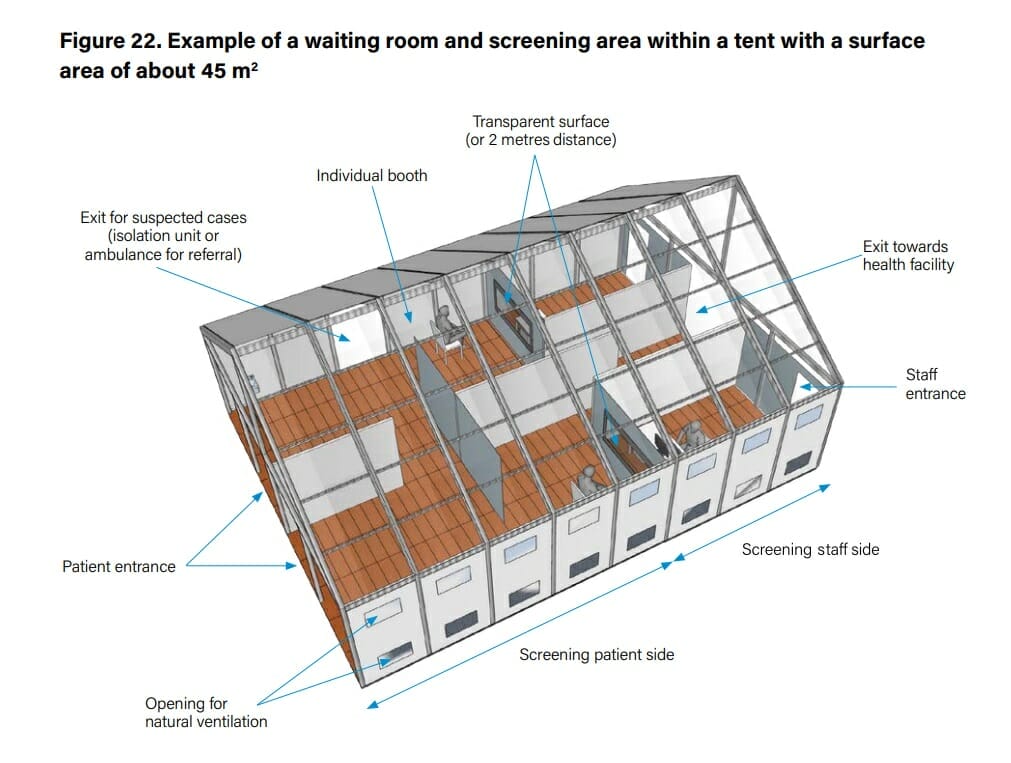
Small tents allow more flexibility in terms of capacity (Figure 22). If required by the epidemiological situation, installing more tents to increase the waiting room capacity or installing a second screening tent can be done easily. Internal separation (screens) can be ensured with wooden frames folded with washable plastic sheeting. The transparent surface for screening can be replaced by a distance of 2 m properly marked, such as a double 1.1 m fence
COVID-19 buildings and tents waiting room and screening area
COVID-19 buildings and tents waiting room and screening area
COVID-19 buildings and tents waiting room and screening area
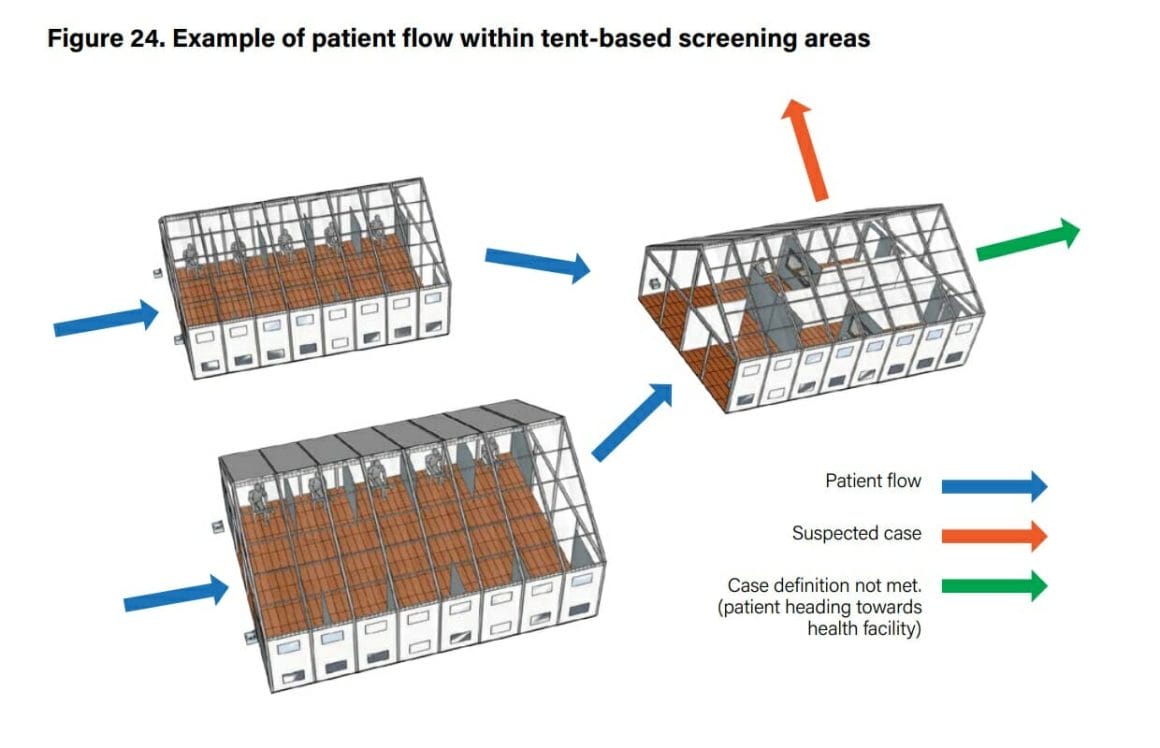
Screening and waiting room tents should be installed correctly to allow clear patient flow, as shown in Figure 24.
Download the WHO standard screening layout for converted buildings and tents.

Other COVID-19 Updates
Tiger Tests Positive for Coronavirus at New York Zoo
Harvard Talks: Cut Salaries or Cut People?
Lamborghini Medical Shields & Surgical Masks for Health Workers
WHO COVID-19 Buildings & Tents Screening Layout Standards
UCLA Engineer Made a Ventilator from Hardware Items
Airbus Gives 3D-Printed Hospital Visors to Health Workers
Airlines COVID-19 Analysis: Aviation Collapsed
Forecast Deaths, Hospitals & Ventilators: COVID-19 Impact, USA Full Report
Ventilation Standards for Buildings Converted to COVID-19 Hospitals
Harvard Talks: The Supply Chain in Post COVID-19 Era
COVID-19 Deaths to Reach 81,000 in US By June – Forecasts by IHME & Univ. of Washington
Top 10 Largest Ventilator Manufacturers in the World
List of Government Officials Tested Positive in PH
Metronic Ventilator Ramping Up Production
Engineers, Can You Help Build a DIY Ventilator for Hospitals?
Water is Our First Line of Defense Against COVID-19
COVID-19 Economic Aftermath on the Construction Industry
Complete List of Companies Working on Coronavirus Vaccine
COVID-19 War: 70K Physicians vs 109M Filipinos
Famous People Who Have Tested Positive for COVID-19
These Politicians Tested Positive for Coronavirus (COVID-19)
Postponed Exhibitions in the Philippines due to COVID-19
Cancelled Major Events Around the World Due to COVID-19
World Bank Gives $12 Billion to COVID-19 Affected Countries
COVID-19 Philippines: DOH on Code Red Status
PPE Shortage Endangering Health Workers Worldwide
The List of COVID-19 Disinfectants Approved by EPA
World Bank Gives $12 Billion to COVID-19 Affected Countries
Air Cargo Demand Down 3.3% due to COVID-19 Disruption
























